February 26, 2026
3 min read
Add Us On GoogleAdd SciAm
Scientists gave the same sample to seven at-home microbiome tests. The results were dramatically different
The science and the regulations to underpin these test “just aren’t there yet,” researchers say
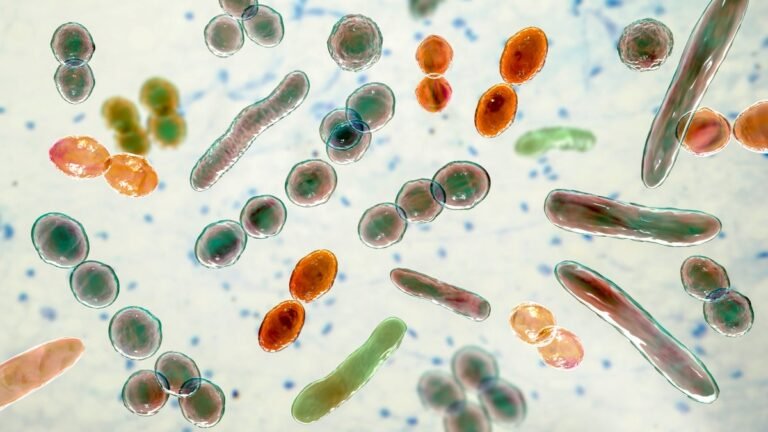
Trillions of microbes help our digestive system function, but testing for them can be a challenge.
Kateryna Kon/Science Photo Library/Getty Images
From drinking celery juice to downing supplements to eating fistfuls of probiotic-rich foods such as kimchi, gut health is high on the wellness agenda. And as you are trying to help your own good bacteria bloom, at-home testing companies that claim to open the black box of digestive health are flourishing.
It’s easy to understand why we have become so captivated by our gut. Scientists have long known that vast colonies of bacteria, viruses and other microorganisms—a population collectively called the microbiome—live on and inside the human body. But how they influenced our health was long a mystery. In just the past few years, we’ve learned that myriad factors, from the food that we consume to the amount of time that we spend sleeping to our genes to our home, all affect our microbiome. And in turn, that can influence our immunity, digestion, and aging and even our emotions.
And that is why at-home microbiome testing has blossomed into a billion-dollar market. But a study published today in Communications Biology suggests some of these tests’ insights might not be as accurate as they claim.
On supporting science journalism
If you’re enjoying this article, consider supporting our award-winning journalism by subscribing. By purchasing a subscription you are helping to ensure the future of impactful stories about the discoveries and ideas shaping our world today.
“The gut microbiome has been linked, at least in the public imagination, to the idea that you can improve a whole range of conditions through diet and lifestyle change,” says Diane Hoffman, a co-author of the study and a health law professor at the University of Maryland, Baltimore. “There’s been a lot of hype around that, but the hype doesn’t really match the evidence.”
According to Hoffman and her co-authors, at-home microbiome tests “straddle the line” between medical and wellness products, placing them in a legal gray area. Currently, there are no microbiome diagnostic tests approved for clinical use in the U.S., even as the market for at-home versions continues to grow.
These direct-to-consumer microbiome tests rely on the user to collect their own stool samples at home—to essentially scoop their own poop into a vial and send it off to a lab for analysis. Stool samples are an effective way to determine which microbes are present in the digestive tract. But different parts of the sample and different ways of storing or processing it can yield dramatically different results. To get a clear idea of how capable at-home tests were, Hoffman and her team created a trial stool sample by blending healthy fecal matter until the mixture of organisms was homogenous throughout.
The research team then randomly selected seven different companies—none of which are named in the study—and collected samples from the same initial fecal source, following the companies’ collection methodology. The team completed and sent back three separate tests to each of the companies. This allowed the researchers to compare the different companies’ results—and to test whether each company’s analysis was precise enough to surface similar results from all three versions of the sample.
The results were even more disparate than the team had expected. Of the more than 1,200 taxonomic groups of microbes identified by all the tests combined, just three microbial genera were present in all seven companies’ results. Even tests processed by the same company didn’t always match.
In one case, a company sent back the results of its three separate tests with two that designated that version of the sample “healthy” and one that designated it “unhealthy.” Such outlier results make the tests’ uncertainties unmistakable, says Scott Jackson, a co-author of the study and a former employee of the National Institute of Standards and Technology. “You can see it stands out like a sore thumb.”
The researchers warn that people who employ these direct-to-consumer tests should not use the results to inform lifestyle changes or medical decisions—especially until the assays are potentially backed by more research and regulation.
“It’s still relatively early as a scientific field,” Jackson says. “I think we will figure it out, but we’re just not there yet.”
It’s Time to Stand Up for Science
If you enjoyed this article, I’d like to ask for your support. Scientific American has served as an advocate for science and industry for 180 years, and right now may be the most critical moment in that two-century history.
I’ve been a Scientific American subscriber since I was 12 years old, and it helped shape the way I look at the world. SciAm always educates and delights me, and inspires a sense of awe for our vast, beautiful universe. I hope it does that for you, too.
If you subscribe to Scientific American, you help ensure that our coverage is centered on meaningful research and discovery; that we have the resources to report on the decisions that threaten labs across the U.S.; and that we support both budding and working scientists at a time when the value of science itself too often goes unrecognized.
In return, you get essential news, captivating podcasts, brilliant infographics, can’t-miss newsletters, must-watch videos, challenging games, and the science world’s best writing and reporting. You can even gift someone a subscription.
There has never been a more important time for us to stand up and show why science matters. I hope you’ll support us in that mission.